Ooof! The low FODMAP diet is a tricky one. But I’ve got you. Hopefully you already read my post ‘What to do before you start the low FODMAP diet‘. (If you didn’t, I highly recommend starting your FODMAP journey there).
Now it’s time to learn how to cruise through the elimination phase of the LFD with the 7 essential tips below.
Getting it right means getting better results. And who doesn’t want that? 😉
1. One intervention at a time
The low FODMAP diet (LFD) is basically a science experiment. You’re testing out whether or not FODMAPs play a role in your symptoms, and if so, which groups you’re sensitive to. Adding another intervention to the mix at the same time, like starting probiotics for example, is like throwing a wrench in the spokes.
When your guts are twisted in painful knots and you look 6 months pregnant by the evening, it’s tempting to throw every possible treatment at the problem all at once. The shot gun approach may bring you some relief, but you’ll be left wondering which intervention actually did the trick.
It’s not worth your time, effort and money to be using treatments that don’t work, so test them out one at a time.
If you truly want to learn about your dietary triggers, don’t start any other intervention while you’re working your way through the low FODMAP diet.
2. Continue keeping a food and symptom journal
I previously discussed the importance of keeping a food and symptom journal before starting the low FODMAP diet to collect baseline data on your usual symptoms.
Tracking your symptoms during the elimination phase will enable you to compare them to your baseline symptoms so you can see if there’s been any improvement.
It’s also wise to note your food and fluid intake during the elimination phase. If your symptoms don’t improve much, you’ll be able to go back and analyze your food record for any issues that may have interfered with your results. This is where a Monash trained dietitian can be incredibly helpful since they know the ins and outs of the LFD and can help you troubleshoot.

Similarly, tracking other health metrics like stress, mood, menstruation, exercise, medications, etc will give you insight into their effect on your symptoms.
3. Use the Monash University FODMAP app
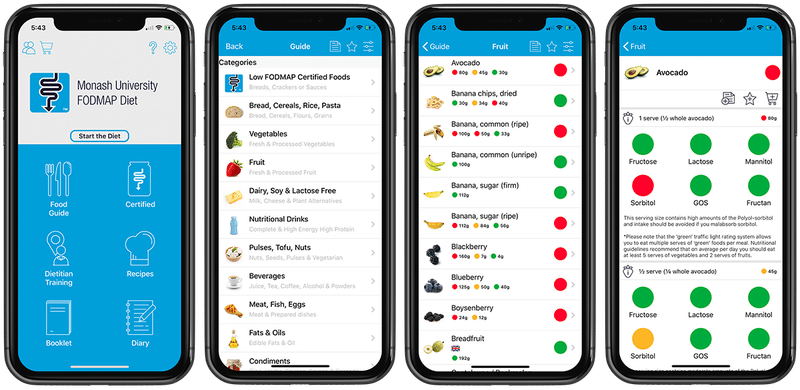
I can’t stress this enough. There are so many FODMAP food lists online that are out of date or just plain wrong. Because Monash University is constantly testing and retesting foods, their FODMAP app is your best source for accurate, up-to-date food lists.
The app uses an easy traffic light system to inform you about the FODMAP content in various foods.
- Green light means low FODMAP at the portion specified.
- Yellow light means moderate FODMAP.
- Red light means high FODMAP.
These food lists increasingly include products from various brands. Many of these items are Australian, but the app is expanding to include brands from Canada, the US and Britain.
More than just listing foods according to FODMAP content, the Monash app also includes:
- General info on IBS and the LFD.
- A food and symptom journal.
- A directory of Monash FODMAP trained dietitians from all over the world.
- Recipes.
- Info on Monash certified low FODMAP foods.
4. Watch your portions
As with any nutrient, the more you eat, the more you get.
The scientists at Monash test the FODMAP content of foods in different portions. It’s common to see a food that is low FODMAP (ie. green light) at a smaller portion, but moderate (yellow) or high (red) FODMAP at larger portions.
White wheat bread is a good example – 1 slice is green, 1.5 slices is yellow, and 2 slices is red. (So yes, you can eat 1 slice of white wheat bread at a sitting).
When eating foods with multiple lights (the little lights under the food name), always stick to the green light portion size. Learn more about low FODMAP serving sizes.
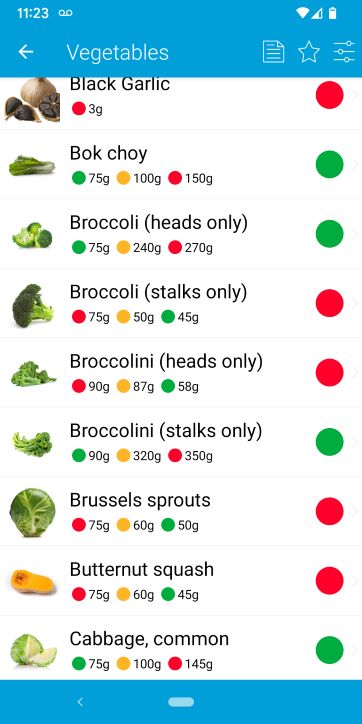
Monash sets its criteria for “low” FODMAP very conservatively, which means you can eat several green light serving sizes at a sitting.
There are some foods, however, with such tiny amounts of FODMAPs that you can eat large portions without worrying about overdoing it. A few examples of ultra low FODMAP foods include:
- brown rice
- arugula, kale, lettuce
- carrots
- cucumber
- potato
- navel orange, clementine
- papaya

5. Eat your fibre

I know, I sound like your mom telling you to eat your veggies, but she was right about that. And I’m right about this.
The low FODMAP diet can improve symptoms of bloating, gas and abdominal pain, but it doesn’t have a great track record when it comes to alleviating constipation.
For those of you with IBS-C, eating enough fibre on the low FODMAP diet is essential to minimize constipation-related symptoms (gas, bloating) from interfering with your results. Unfortunately, the LFD can be a bit low in fibre so check out my blog post ‘Low FODMAP High Fibre Foods‘ for info on which foods to eat.
Fibre benefits all folks with IBS, regardless of subtype, by:
- Nourishing the microbiome.
- Increasing short chain fatty acid production by intestinal bacteria.
- Improving cholesterol.
- Lowering blood sugars (1).
6. Stay organized with a meal plan
I wish I could tell you that the low FODMAP diet is a piece of cake (pun intended) but it isn’t so I can’t. That’s why I highly recommend connecting with a Monash trained dietitian to guide your through the diet, or at least turning to sources of credible info (like this blog – shameless plug) that I outlined previously.
Making a meal plan may sound like a lot of work upfront, but it’s entirely worth it to make your life easier and keep you on track with the diet.
Benefits of a meal plan:
- Helps you create your grocery list.
- Having a grocery list saves you money via precision shopping.
- You spend less mental effort during the week figuring out “what’s for dinner tonight?”
- You can plan leftovers for lunch or cook-free evenings.
- You always have a game plan so you’re less likely to order take-out.

7. Minimize eating out or buying pre-made food
Don’t worry, I’m not asking you to completely cut out resto dining. I’m merely suggesting that you limit – ie. reduce to a minimum – eating out in order to control your FODMAP intake during the elimination phase.
When you’re eating at restaurants, ordering take-out or buying pre-prepared foods, it’s really hard to control your FODMAP intake for a number of reasons.
- It may not always be possible to swap out high FODMAP foods for low FODMAP alternatives.
- Garlic and onion are in everything! They’re foundational flavourings that add depth and flavour to many a dish.
- Portions tend to be large so it’s easy to overdo it on the FODMAPs.
Remember: the low FODMAP diet is short term. Once you have a handle on which FODMAP groups trigger your symptoms, you can be strategic with your restaurant choices and eat out with a lot more freedom and ease.
In summary, if you want to kick ass on the low FODMAP diet and truly learn how foods affect your symptoms, follow these 7 tips during the elimination phase:
- One intervention at a time.
- Continue keeping a food and symptom journal.
- Use the Monash FODMAP app.
- Watch your portions.
- Eat your fibre.
- Stay organized with a meal plan.
- Minimize eating out.
As always, drop me a line in the comments section if you have any questions.
xoAndrea, RD



